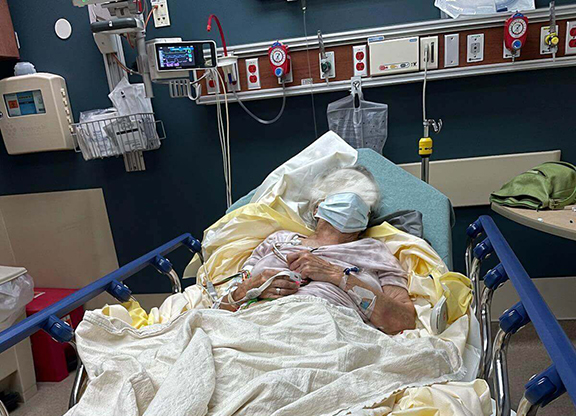
The Result of Intensive Advocacy & Care
| Late in the afternoon on Friday June 24th the police found Ms. L. sitting on a bench dressed in her fluffy pink robe, slippers and nightgown. Her only possessions were a purse and a large plastic bag from a local hospital. Ms. L. had discharge paperwork from 4 Emergency Department visits in the bag, one carried a diagnosis of malingering. The police were incredibly kind, one even paid for her lunch, but they were stumped. They had no where to take her. “Malingering is falsification or profound exaggeration of illness (physical or mental) to gain external benefits such as avoiding work or responsibility, seeking drugs, avoiding trial (law), seeking attention, avoiding military services, leave from school, paid leave from a job, among others.” – National Library of Medicine There was no point in taking her to the hospital again, and she definitely didn’t belong in prison. So what to do? |
| They couldn’t take her to a congregate shelter; there are rarely ever any beds on a Friday night, especially a bottom bunk that is mandated for anyone over 55 years old. She had already tried that and she was too afraid to go back. About that time Amie Zamudio, the co-founder of Housing 4 the Homeless, spotted them and approached. One of the officers who knows about the work that Amie does, asked, “can you please help this woman?” This is a question that we get from a wide variety of professionals who are desperate to help but have no options. We are contacted by physicians, county workers, psychiatrists, Adult Protective Services workers, outreach workers from other non-profits, activists, Cal-Aims staff, and concerned citizens all the time. Even the HOT Team has asked us if we can provide a room for people they find on the streets. |
H4H Intervention
1) First, we settled Ms. L. into a room of her own, with a private bathroom, a microwave, mini fridge, and most important of all a locking door.
2) The next day, after she had a chance to get a good nights sleep, we enrolled her into our Emergency Shelter program, entered her into the Homeless Management Intake System, and arranged for an appointment with a primary care physician.
3) Simultaneously Amie started putting together the pieces of her life. She found her former landlord, family members, and where her things are stored.
WE DISCOVERED THAT HER LANDLORD HAD DUMPED HER AT ALVARADO HOSPITAL – PUT HER THROUGH THE PROCESS OF SELF- EVICTION AND HAD PUT HER THINGS IN STORAGE, ALL WITHOUT HER PERMISSION
4) It became clear that Ms. L. was experiencing an extreme level of anxiety. She paced up and down the hallways in her bathrobe telling everyone that she was afraid.
5) Amie tried to make an appointment with a mental health professional, the soonest in person mental health appointment was December; they settled for Tele-Health which was two weeks out.
6) A local agency that works with seniors with mental health issues had a two month waiting list for an initial intake interview.
7) We contacted County Behavioral Health and Jane Westin mental health centers and they both said that it sounded like Ms. L. was suffering from Cognitive Impairment so they would not be able to help her or proscribe anxiety medications because cognitive impairment is a health issue.
8) We contacted UCSD Senior Behavioral Health Center, they said that they weren’t doing assessments on site due to COVID so the only way she could get in line for a bed would be to take her to the ER.
It became clear that Ms. L. needed a much higher level of care than we were able to provide but there was literally no where for her to go.
At this point, having no other options, Amie took her back to the Emergency Department hoping to get a Cognitive Assessment. Despite a psychiatrist at the hospital referring her to the Neurology department and requesting a cognitive assessment, and Amie advocating very strenuously on her behalf, the doctor on the next shift discharged her once again with three Ativan and a recommendation to see a therapist.A few days later
Ms. L. wanted to go to the local store, she did not want a walker and didn’t want a ride. Worried for her safety Amie followed her.
Unfortunately she fell in front of the store and ended up back in the hospital with physical injuries!
This time Amie was able to convince staff that they could not discharge her again without a plan. She made it clear that she would hold them personally responsible if anymore harm came to Ms. L. They agreed to keep her but they still refused to do a cognitive assessment.
In the meantime Amie had tracked down Ms. L.’s only living relative, a sister living north of LA. Amie coached her in what to say; as a family member she was able to demand a cognitive assessment.
FINALLY, on August 17th, after eight weeks and six emergency room visits Ms. L. was properly diagnosed with Senile Dementia. They verified what we knew all along, she needed intensive support and care. She wasn’t in fact malingering, she was no longer capable of caring for herself.
The Happy Ending
On September 8th Ms. L. was transferred to a custodial Skilled Nursing Center.
Her journey isn’t over yet, but thanks to Amie she’s safe for now and getting the care that she so desperately needs.
It took 76 days – 6 trips to the ER – 3 weeks in a hotel room – 55 days in the hospital Intensive personalized care and advocacy to get Ms. L. to safety
Please help us to continue to provide this level of care by donating your time and or your resources to H4H